Oral Manifestations of Psoriasis
While lesser known than psoriasis of the skin (cutaneous psoriasis) psoriasis-related conditions in the mouth do afflict some people. It’s not easy to diagnose or remedy. There are a limited number of studies that have investigated the oral manifestations of psoriasis.
Can psoriasis occur in the mouth?
Psoriasis is an autoimmune condition of the skin that causes cells to grow and reproduce faster than usual. This causes the creation of plaques, thickened red or sometimes silvery patches that look like scaly spots on the surface of the skin.
The scaly skin associated with psoriasis tends to appear on the hands, knees, elbows, groin area, and scalp, but can also cause lesions on mucous membranes, including the tongue, lips, and areas inside the mouth. Those include the gums, palate, and cheeks.1,2
What is oral psoriasis?
Psoriasis in the mouth is uncommon, some might call it controversial, questioning whether it is a distinct condition,2 Certain changes in the mucous membranes of the tongue and mouth have been associated with some psoriatic subtypes including pustular psoriasis or erythrodermic psoriasis.
Oral symptoms appear to share similar cellular features with the related skin condition, and often follow a clinical course that occurs along with skin manifestations.2
What are the symptoms of psoriasis in the mouth?
Changes in the mouth are typically clinically subtle and can difficult to recognize. When looking inside the mouth, a dentist or dermatologist should consider other conditions.
A clinical diagnosis for oral psoriasis can be extensive and include ruling out a variety of other inflammatory, ulcerative, blistering, and infectious conditions. Mucosal abnormalities can be caused by poorly fitted dentures or other prostheses, chronic cheek biting, or smoking. Those conditions may look like oral psoriasis.2
What does the research say about oral psoriasis?
There is no reliable incidence rate for psoriasis in the mouth.2 This is because the oral cavities of psoriatic patients are rarely examined and biopsies are generally not taken, so the condition may be underreported.
Also, cells of the mouth turn over quickly, and affected cells may not be present at the time of the investigation. Observations suggest that a common inflammatory process may contribute to the development of both psoriasis and periodontal disease.2 Standard treatment approaches for psoriasis on the skin surface are typically not appropriate for treatment inside the mouth.
Understanding how the surface of the tongue functions
The tongue’s surface is covered with papillae (small sensory hair-like projections) and taste buds. They go through a normal shedding process. They also help to balance the microenvironment of the mouth and in so doing help keep our mouths moist, healthy, and infection-free. When the mouth gets infected papillae to help to fight off infection.3-5
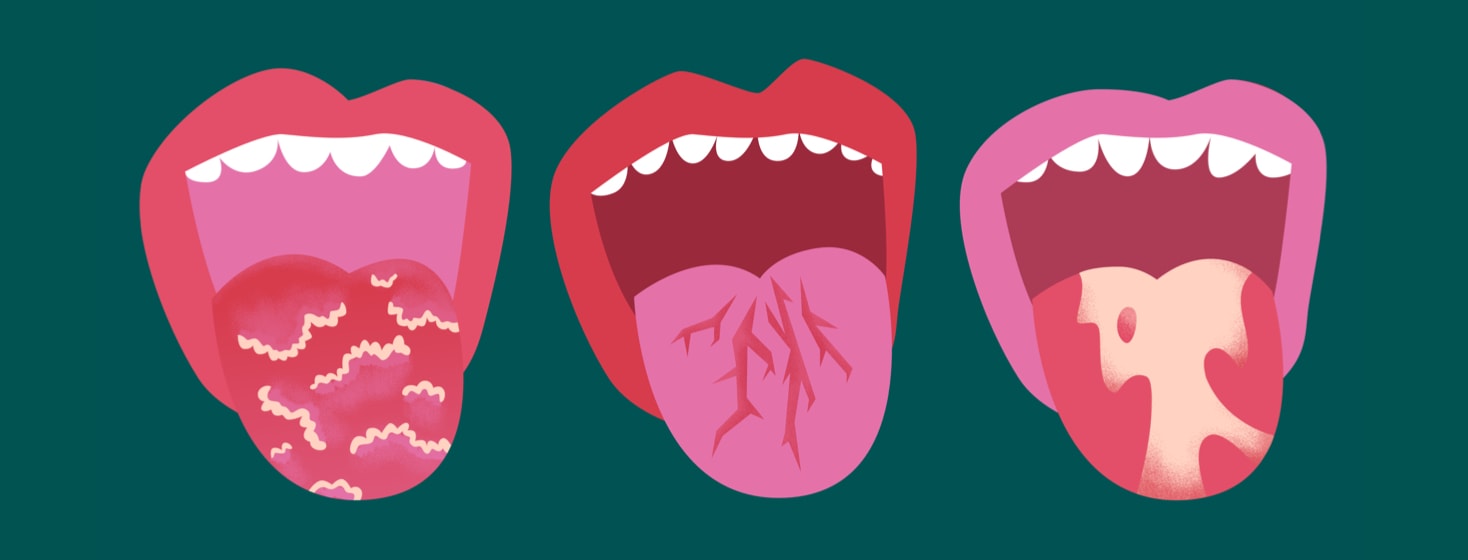
Sometimes the shedding process happens too early or unevenly. This can create sore areas accompanied by white or red patches (geographic tongue), sometimes with fissures, that is deep cracks or grooves on the surface of the tongue (fissured tongue).4
What are fissured and geographic tongue?
In one recent study, investigators sought to identify any correlation between a fissured tongue (FT) and psoriasis severity and age of psoriasis onset. The results: FT is associated with late-onset psoriasis but not with the psoriasis severity.1
The clinical features of the fissured or geographic tongue (GT) are generally benign, just an inflammatory condition that affects the tongue’s surface. Discoloration and patchy areas can be found on the surfaces of a geographic tongue. The irregular markings often resemble a map.4
Research examining geographic tongue and psoriasis
Researchers have looked at the clinical markings of a geographic tongue (GT) to identify and understand the correlation with psoriasis.3 They conducted examinations of the oral cavity in people with and without psoriasis to identify any burning sensation; the number, classification, and location of lesions; loss of papillae; severity of GT lesions; and association with fissured tongue (FT).3
The analysis showed significant differences between the groups with and without psoriasis as related to gender, presence of burning sensation, and severity of geographic surface. Yet study findings concluded that some GT cases may represent true oral psoriasis and some cases may just be GT. Thus, any connection between geographic tongue and psoriasis requires further investigation.
Having your mouth examined routinely
For people with psoriasis, routine skin exams by a dermatologist should include the mouth, looking at the oral mucosa in order to identify subtle changes which could represent oral psoriasis.2
Routine dental exams should also consider the changes in the condition of the oral cavity including the tongue and gums, looking for symptoms that are consistent with oral psoriasis. This could improve the capturing of more accurate incidence reporting.
Treatment of oral psoriasis
Not a lot is written about the treatment of oral psoriasis because most cases don’t require specific intervention. A change in the appearance of the tongue may be bothersome to some people. Symptoms such as burning, pain or changes in perception of taste may fluctuate along with flare-ups of the skin condition.
There are topical steroids and retinoids that are sometimes prescribed and other systemic medication options available for severe cases. A doctor or dentist can offer the best advice on appropriate treatment, if needed, after confirming a diagnosis.2,6
Join the conversation